Feeding 'normal hospital food' to patients with serious illness may increase the risk of death

When you hear 'hospital food,' you tend to think that nutritional balance and calories are calculated perfectly, but the nutritional distribution of hospital food is not always excellent, and
Individualized Nutritional Support for Hospitalized Patients With Chronic Heart Failure --ScienceDirect
https://www.sciencedirect.com/science/article/abs/pii/S0735109721009384
Hospital Food Is Never Great, But For Some Patients It Means Death
https://www.sciencealert.com/for-those-with-chronic-heart-failure-hospital-food-really-can-kill-you
Hospital food provided to inpatients is chopped or boiled to make it easier to eat, but many nutrients are lost during this cooking process. In addition, many patients cannot eat enough due to loss of appetite, and as a result, they tend to lack nutrition and calories during hospitalization. According to a 2019 study , more than 30% of patients in the United States are at risk of malnutrition during hospitalization.
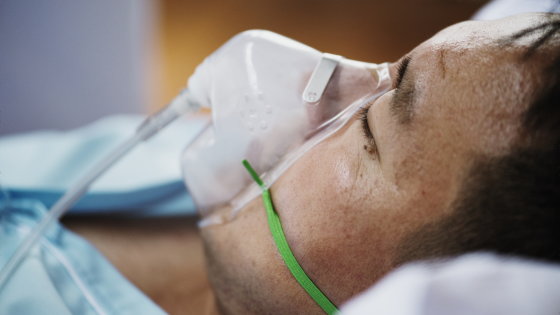
So a Swiss research team conducted an experiment with 645 patients hospitalized for chronic heart failure to investigate the effects of hospital food on the health of inpatients. Chronic heart failure is a condition in which a problem occurs in the heart that acts as a pump that pumps blood to every corner of the body, and the condition of not being able to pump enough blood continues and progresses for a long period of time. Chronic heart failure is known to have a very poor prognosis because it is the terminal condition of all heart disease.
In this experiment, hospitalized patients with chronic heart failure were randomly classified and one group was provided with nutritional support by a certified dietitian within two days of admission. Dietitians created menus with calorie, protein, and micronutrient intake goals and tested them every day or two to see if they were achieving their nutrition goals. In addition, at the time of discharge, he provided dietary counseling and dietary supplements as needed. On the other hand, the other group, which was the control group, was not supported by a dietitian and was provided with the same hospital food as usual.

As a result of the experiment, 27 out of 321 patients (8.7%) who received dietitian intervention died 30 days after admission, whereas 48 out of 324 patients (8.7%) in the control group were provided with hospital food. 14.8%) died. In other words, patients fed a regular hospital diet were nearly 1.7 times more likely to die within 30 days than patients who received careful nutritional support. The same trend persisted thereafter, with one-quarter of patients in the intervention group dying by 180 days, compared with one-third of patients in the control group.
It seems that the average length of stay of inpatients was about 10 days, but considering that nutritional support at the time of admission affects the long-term patient mortality rate, patients in the intervention group are discharged at a certain rate or more. It is suggested that he continued to follow the nutritionist's instructions and continued to eat with careful nutrition. In addition, although it is not specified what was the problem with the hospital food in this experiment, it is possible that lack of nutrients and calories, or excess salt and excess fat had an adverse effect.
'Our study does not provide evidence of the effects of a single nutritional component. Rather, the overall strategy of providing nutritional support to achieve different nutritional goals during hospitalization is a chronic heart failure. It suggests that it is beneficial to the patient. '

Related Posts: